 (212) 861-9797
(212) 861-9797
 (212) 861-9797
(212) 861-9797
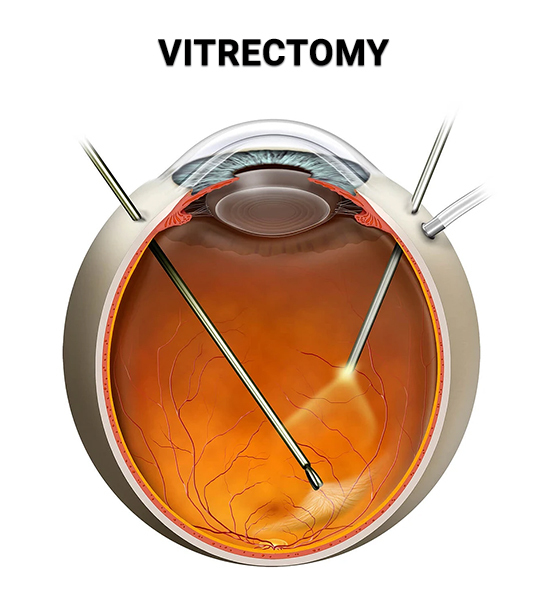
Vitrectomy is a microsurgical procedure used to treat certain retinal disorders such as macular hole, macular pucker, retinal detachment, proliferative diabetic retinopathy, intraocular infections, and traumatic eye injuries. Using specially designed instruments and techniques, vitrectomy specialists perform the procedure by removing the vitreous gel through a very small incision in the eye wall. The vitreous gel is replaced with a saline solution. Then, using a high-intensity fiber optic light source, your surgeon will use a specially designed microscope that provides a clear view of the vitreous cavity and retina at different magnifications to perform any additional work if necessary, such as removing scar tissue (macular pucker, tractional detachment) or closing a macular hole. This same-day surgical procedure is usually performed by a retina specialist under local anesthesia and intravenous sedation.
Considering the importance of vision and the numerous serious diseases which pose a life changing threat, there is no room for error. The finest eye specialists in the country are found at VRMNY. I have been a patient there for decades and have been seen by several doctors. They define the meaning of expert and consult with one another to ensure accuracy. The office is spotless. The staff is courteous and professional. The visits are usually time consuming due to the necessity of imaging and a preliminary exam with a technician before seeing the specialist. I consider myself fortunate and am very grateful to be a patient there.
RENEE B. GoogleOur vitrectomy doctors have developed and patented specialized tools to make the procedure more precise and less traumatic, including flexible probes, endoscopic systems, and electromagnetic detectors. These innovations enable surgeons to perform even the most complex cases, particularly when the retina is difficult to access or visualization is limited.
To achieve the best possible outcome, your surgeon may use several specialized techniques, including:
These gases are used to flatten a detached retina and keep it attached as healing of laser or cryopexy (freezing) around retinal tears occurs. Gas is also used to close macular holes. The advantage of intraocular gases is that the body absorbs them over the course of several weeks. Until about 50% of the gas instilled into the eye has disappeared on its own, vision is usually limited to the level of hand motions. Patients must avoid travel to high altitudes and flying as long as the gas is still in the eye, because gas will expand under those circumstances and can cause dangerously high pressures in the eye. Also, patients usually will be required to keep their head in a certain position for an extended period of time to ensure the success of the treatment. Possible short- and long-term complications of intraocular gas are cataracts and glaucoma.
In some instances, silicone oil is used instead of intraocular gases, particularly when long-term support of the retina is needed. In contrast to the intraocular gases, silicone oil remains in the eye indefinitely unless it is surgically removed. Usually the oil is left in place for several months, but in certain instances it may desirable to keep it in the eye for years. Vision is less affected by the silicone oil compared to intraocular gases. Positioning is less critical, making this procedure more conducive for children and the elderly with neck or back problems. Risk factors include cataracts and glaucoma as well as possible damage to the cornea.
Lasers are often used during vitrectomy eye surgery to surround retinal tears and prevent future leakage of vitreous fluid under the retina. Laser is also used to treat damaged retina in proliferative diabetic retinopathy.
There are several instruments used to remove scar tissue and foreign bodies such as forceps, scissors, and picks. There are hundreds of vitrectomy instruments available to assist surgeons. Most vitreoretinal tools are smaller than 1mm in diameter, making them some of the most precise and finely crafted instruments available today.
This is a technique used on its own to repair a retinal detachment or combined with a vitrectomy surgery to offer additional support in reattaching the retina. Learn more about the scleral buckle procedure on the Retinal Detachment page.
A lensectomy is often performed when a cloudy natural lens (cataract) prevents the surgeon from clearly viewing the ocular structures behind it. It involves surgically removing the eye’s crystalline lens during the eye vitrectomy procedure. In some instances, a lensectomy may also be necessary to remove scar tissue during more complex retinal detachment procedures. The lens can be replaced with a clear lens implant either during the same surgical procedure or at a later date.
Several risks involved include bleeding, cataracts, glaucoma, detachment or re-detachment of the retina, and ultimately vision loss. We will thoroughly discuss your treatment and potential risks involved so you can make an educated decision about your treatment.
Vitrectomy is one of the most complex and delicate procedures in ophthalmology, and it has been a central focus for the physicians at VRMNY for decades. This is not just routine surgery here. Our vitrectomy doctors handles a full spectrum of vitreoretinal cases, from common floaters to the most advanced retinal detachments and macular disorders. Many of the surgical approaches and refinements now standard in the field were influenced by the work of our doctors.
Several of our physicians hold faculty appointments at Lenox Hill Hospital, New York University, and the New York Eye and Ear Infirmary. In these academic roles, they teach future ophthalmologists, lead surgical training programs, and contribute research that shapes modern retinal surgery techniques worldwide. Their involvement keeps our team at the leading edge of both technology and clinical practice.
Among our specialists:
Dr. Richard F. Spaide, MD — Known worldwide for advancing fundus autofluorescence and high-resolution OCT imaging. These tools are vital for planning tricky vitrectomy surgeries, like those for macular holes and epiretinal membranes. His work gives surgeons clear, detailed information before surgery, helping improve results everywhere. He’s also created and patented several key instruments used in vitreoretinal surgery.

Dr. Michael Engelbert, MD, PhD — A leading expert on the vitreous and vitreoretinal interface. He focuses on small-gauge vitrectomy techniques that make surgeries less invasive and speed up recovery. His surgical skills, research, and talks have helped shape today’s methods for treating vitreoretinal diseases.

Dr. Yale L. Fisher, MD — A pioneer in using ocular ultrasound and endoscopy for retinal surgery. These tools allow surgeons to see through obstacles when the retina is hard to view—crucial for safe vitrectomy. He’s also developed new surgical methods and instruments that still impact the field today.

The combination of advanced diagnostics, refined surgical skills, and direct access to cutting‑edge equipment allows VRMNY to handle cases that many practices refer elsewhere. With a state‑of‑the‑art retina center in Manhattan and additional offices serving the greater New York Metropolitan area, VRMNY is the largest retina‑vitreous practice in the region — and one of the most experienced teams performing vitrectomy anywhere in the country.
Vitrectomy surgery typically takes between 30 minutes to 2 hours, depending on the complexity of the condition being treated. The duration may vary based on factors like the severity of the retinal issue and whether additional procedures, such as membrane peeling or laser treatment, are required.
After a vitrectomy, it is crucial to follow post-operative care instructions to ensure proper healing. Avoid:
If a gas bubble was inserted during surgery, flying is strictly prohibited until the bubble dissolves, which can take 2 to 8 weeks, depending on the type of gas used. Flying too soon can cause the bubble to expand, leading to severe complications, including vision loss. Always consult your ophthalmologist before planning air travel.
Vitrectomy surgery can be performed under:
As best-in-class New York vitrectomy specialists, the doctors at Vitreous Retina Macula Consultants of New York provide highly personalized and comprehensive eye care. They have earned some of the most respected reputations in the United States. For more information about the vitrectomy procedure in NYC, including advances in instrumentation, techniques, and the treatment of vitreous and retinal diseases, schedule a consultation with one of our specialists.
Let us help you enjoy your life
Call: (212) 861-9797To Speak With An Appointment Coordinator Now